 While the current monkeypox outbreak has raised new awareness of the disease in Western countries, previous outbreaks in Africa attracted little attention globally. Dr. Dimie Ogoina, an infectious diseases physician in Nigeria, along with his team at Niger Delta University Teaching Hospital, diagnosed and managed the first reported case of monkeypox during the country’s 2017 outbreak. He describes the history of the disease in Nigeria, remaining questions and what’s needed now to address it in Africa.
While the current monkeypox outbreak has raised new awareness of the disease in Western countries, previous outbreaks in Africa attracted little attention globally. Dr. Dimie Ogoina, an infectious diseases physician in Nigeria, along with his team at Niger Delta University Teaching Hospital, diagnosed and managed the first reported case of monkeypox during the country’s 2017 outbreak. He describes the history of the disease in Nigeria, remaining questions and what’s needed now to address it in Africa.
On April 4, 1971, a 4-year-old girl living in Ihie-Imuduru village in Abia State, South-East Nigeria, developed a febrile illness associated with generalized vesiculopustular skin lesions. Nine days later, her 24-year-old mother also developed fever and skin rash. Following laboratory investigation, the child was confirmed as the first human case of monkeypox in Nigeria, while the infection in her mother was reported as the first suspected human-to-human transmission of monkeypox in history.
Both mother and child were unvaccinated for smallpox, but the source of the child’s infection was unknown, as there was no prior contact with animals or contact with a suspected case of monkeypox 21 days preceding her illness. None of the more than 300 contacts, including 12 unvaccinated household contacts, developed symptoms of monkeypox. However, asymptomatic infection was not investigated.
No other case was reported in the country despite active surveillance until November 1978, when a third case was diagnosed in Omifounfoun village in Oyo State, South-West Nigeria. The patient was an unvaccinated 35-year-old traditional herbalist who became ill while temporarily living in Omifounfoun but later travelled to his hometown in Benin Republic, where monkeypox was confirmed by viral isolation. The source of infection was unknown, although he occasionally consumed bush meat, like other members of his household. After an extensive search, no secondary case was detected either in Nigeria or Benin Republic, even among unvaccinated contacts. Between 1971 and 1979, several attempts to identify animal reservoirs of the monkeypox virus in Nigeria were not successful.
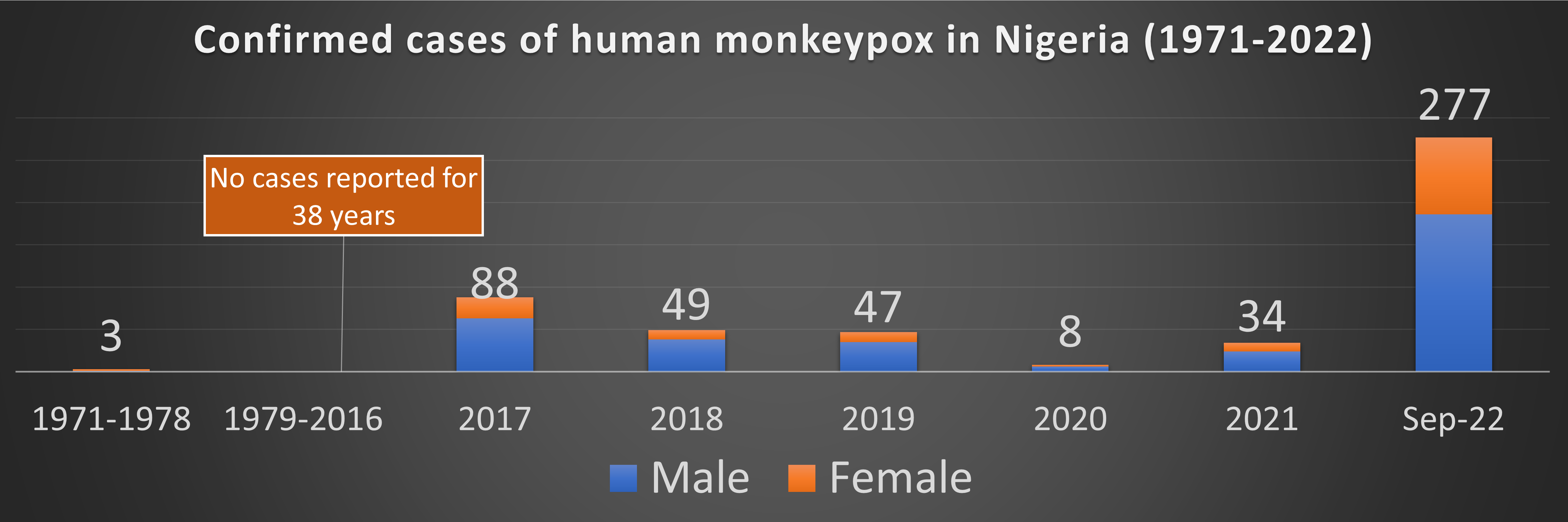
New cases reported in 2017
On the evening of Sept. 24, 2017, an 11-year-old boy was referred to Niger Delta University Teaching Hospital, in Bayelsa, Nigeria, with a diagnosis of atypical chickenpox. Managing clinicians suspected monkeypox, and the skin swab later returned positive for the monkeypox virus. This was the first time since 1978 Nigeria had reported a case of monkeypox. In the following weeks, many more cases were diagnosed across Nigeria, and in contrast to prior outbreaks from Africa, most of the affected population were urban dwellers and young adult males.
Of 122 confirmed cases reported as of September 2018, 8% reported animal contact, 9.8% had close contact with a confirmed case, and more than 70% had no known source of exposure. The 12 close contacts of confirmed cases included one prison inmate, two health care workers who participated in the management of cases and nine household contacts, five of whom were family members of the index case.
The 35-year-old uncle of the index case was the first to develop symptoms in the household. His symptoms were mild, associated with a genital rash, and he reported unprotected sex with a female sex worker before onset of his symptoms. Between 2017 and 2021, 226 laboratory-confirmed cases and eight deaths (3.5% case fatality rate) due to monkeypox were reported in Nigeria. A prior study from Nigeria had reported more severe disease and deaths among monkeypox-HIV-coinfected cases with significant immunosuppression. While the source and modes of transmission of monkeypox were largely unknown, transmission via sexual contact was proposed among a cohort of cases with genital ulcers, concomitant HIV and syphilis infections, and associated high-risk behaviors, including multiple heterosexual partners.
Current global outbreak and response
The period between 2018 and 2021 was characterized by exportation of monkeypox from Nigeria to parts of Europe and the USA by international travel. Then, on May 13, 2022, a cluster of cases of monkeypox, mostly among gay and bisexual men who reported multiple sexual partners, was reported in parts of Europe without any travel link to African countries where monkeypox had occurred historically. The unprecedented outbreak was due to the same strain of virus (Clade 2) causing disease in Nigeria, although evidence suggests genomic mutations might have made the virus more adaptable to the human host.
As of August 2022, more than 50,000 cases have been reported in more than 100 countries in all continents of the globe. Although likely to be a gross underestimation, as of September 2022, Nigeria has reported more than 300 cases and four deaths in 2022 alone, which is higher that the cumulative number of cases reported in the prior five years. However, the source of infection, modes of transmission, risk factors for infection and natural history of the disease in Nigeria in 2022 are yet to be defined. Consequently, investments in surveillance and research should be prioritized to address knowledge gaps regarding monkeypox in Nigeria.
Regrettably, two months after monkeypox was declared a public health emergency of international concern, Nigeria, like other affected African countries, has yet to receive a single dose of monkeypox therapeutics or vaccines, even for clinical trials. As cases decline, especially in the global north where medical countermeasures are widely available, it seems monkeypox, like HIV, will again be forgotten as a disease for Africa and other minorities, unless the world urgently acts in global solidarity to prevent history from repeating itself.


